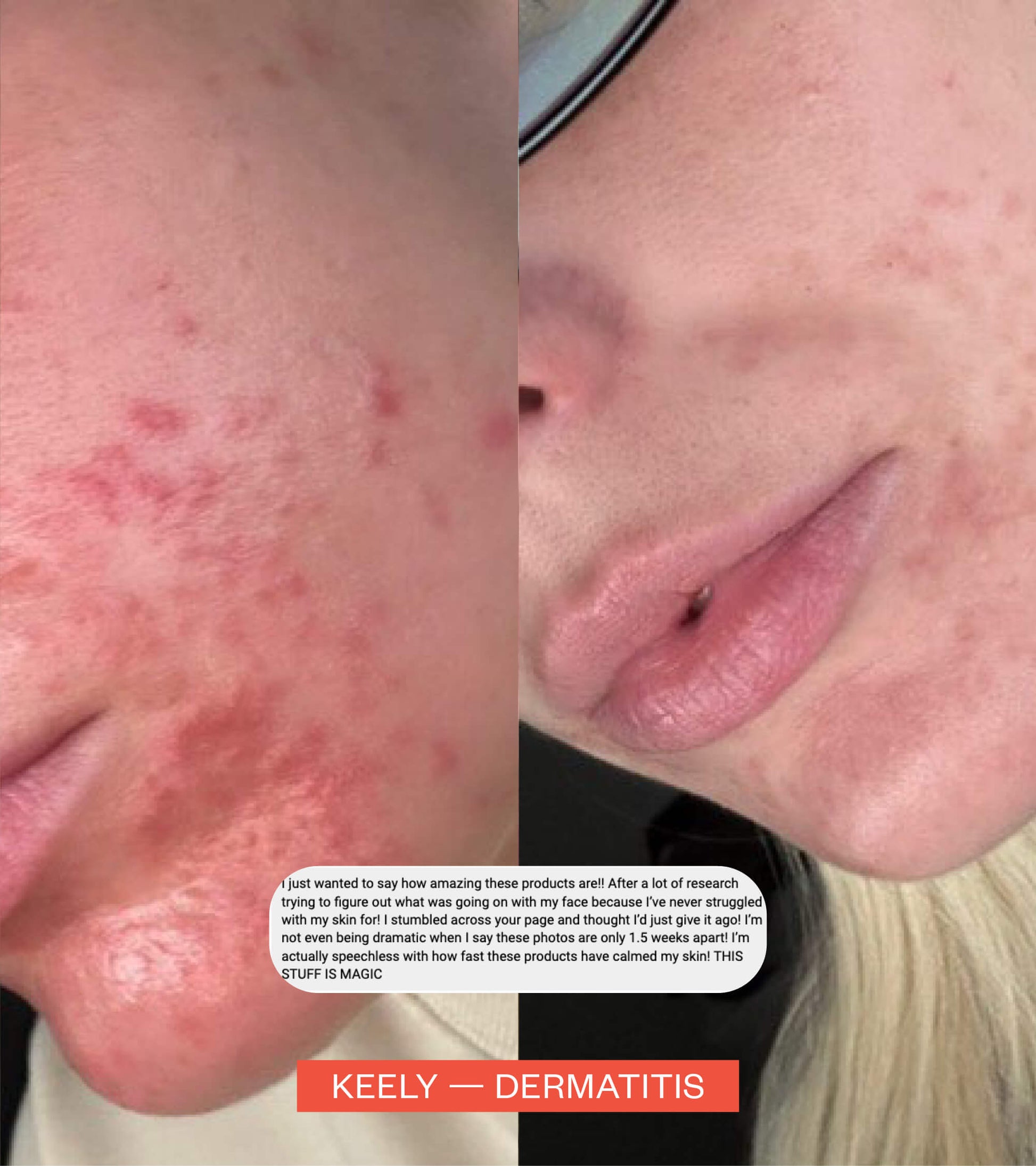
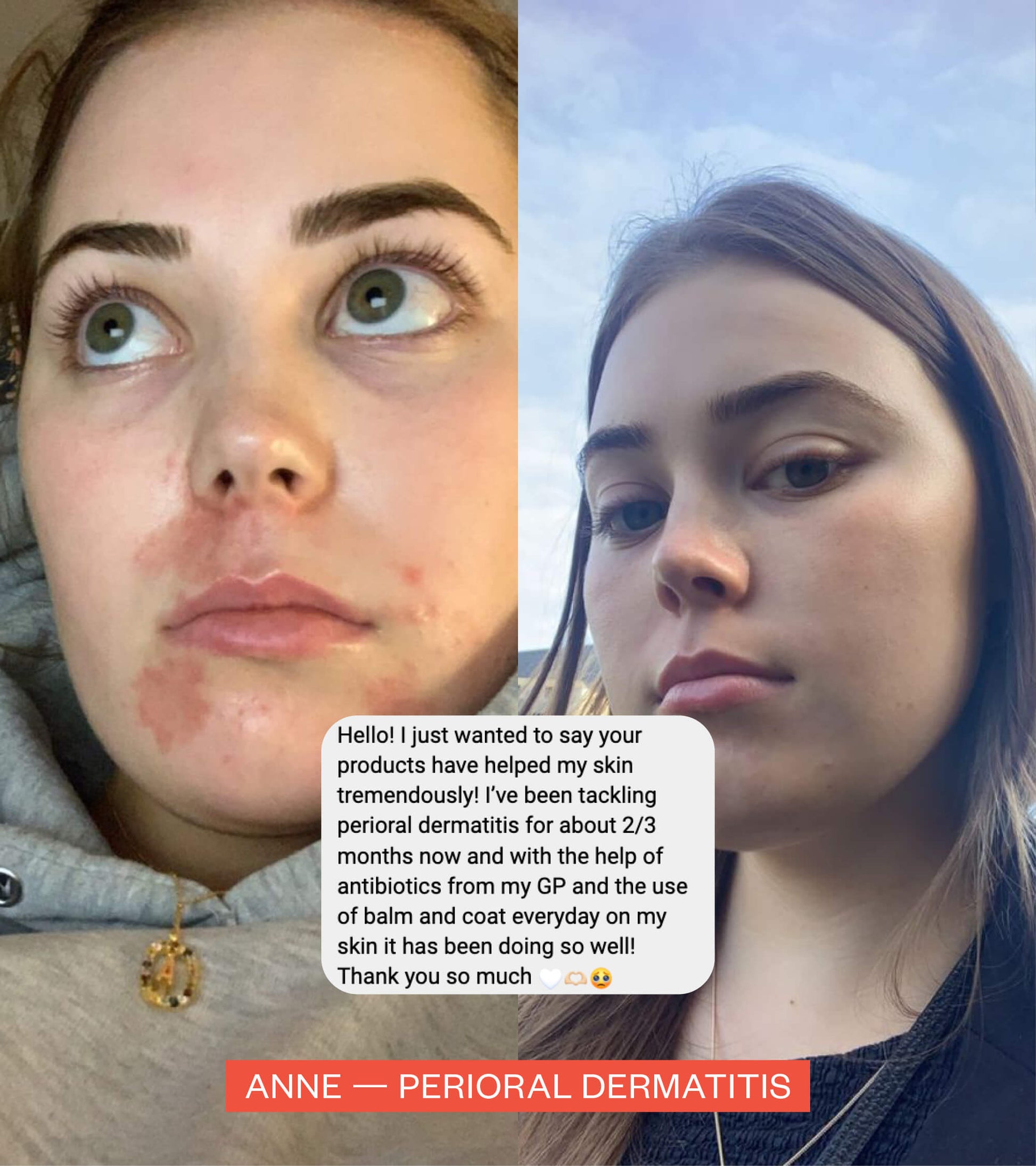
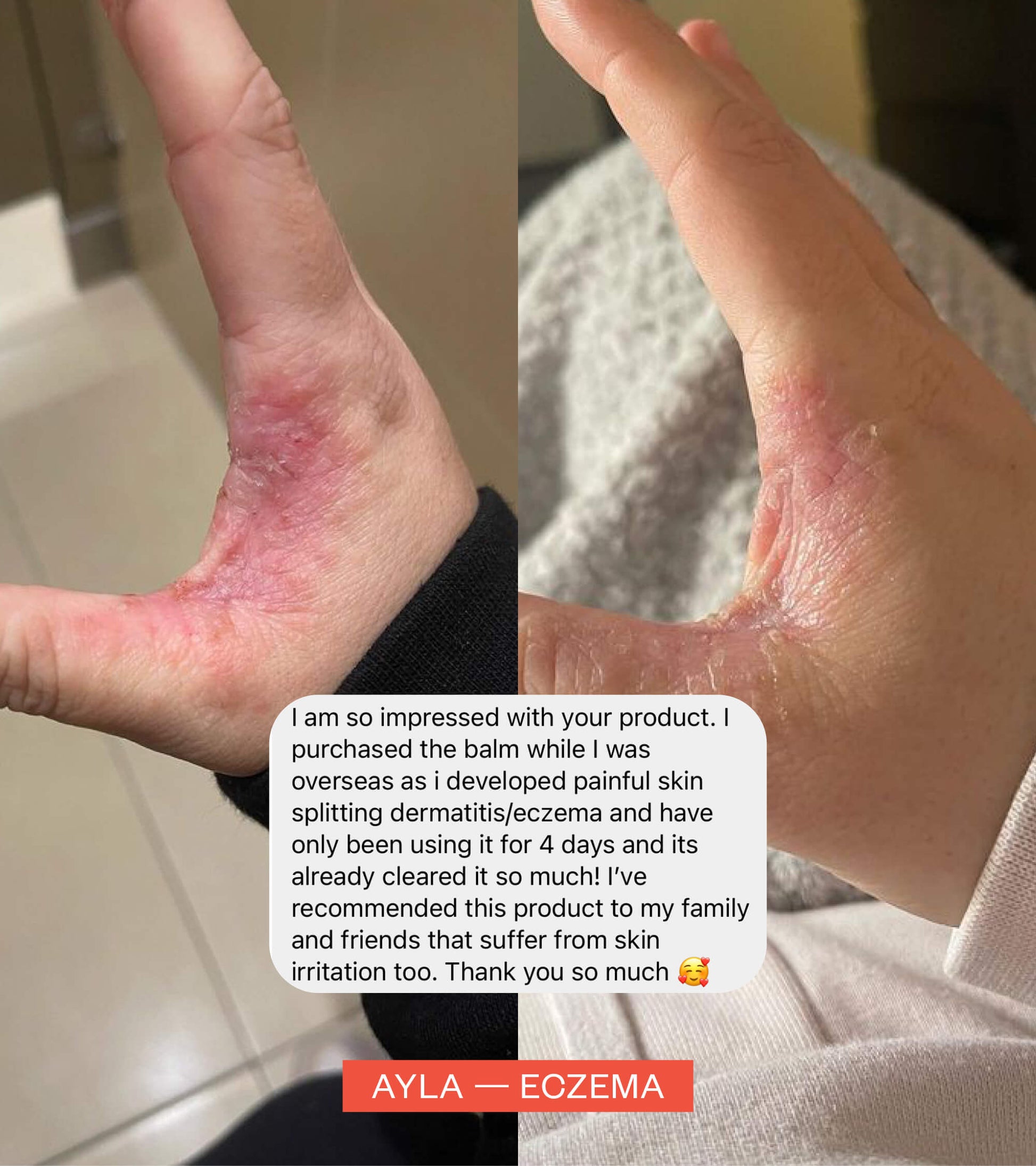
Jess — A psychologists’ experience with Postnatal Depression and anxiety
Being a woman is both beautiful, and challenging, and our bodies go through so much to bring little humans into the world.
Trigger warning: this talks about suicidal thoughts and depression.
As part of our Mother’s Day campaign Sensitive Mothers, we spoke to psychologist Jess about her experience of postnatal depression and anxiety after the birth of her beautiful boy, Rio.
In March 2020 Jess gave birth to a beautiful baby boy, Rio. If you remember that time (many of us would like to forget), it was the start of lockdown in Melbourne. Jess always wanted to be a Mum, but never expected to bring a little human into the world this way — in a hospital surrounded by people with masks and funny protocols. On top of that, her birth did not go as she imagined. It started well and naturally, yet ended up being an emergency c-section, followed by slow healing and lots of meds for pain management. Postpartum care was also not a thing due to COVID protocols, so from the get-go, she felt isolated, even being in a beautiful baby love bubble with Rio, and her husband.
Jess’ family lives by the coast, and her partner is from Italy, so when the sleepless nights and anxiety started to kick in there was very little family support she could turn to. Motherhood did not come easily as she thought it would — why was it so hard? Was there something wrong with her? How could she escape? Jess felt so much guilt all the time. Postnatal anxiety and depression presented as intrusive thoughts about harm coming to her baby, spiraling when she couldn’t sleep, and painful reminiscing about the simplicity of pre-baby life. She kept thinking ‘what have I done?’ which of course led to guilt. Her stomach was always churny, she lost her appetite, then there was the brain fog, weight loss, and low milk supply.

At around four months postpartum, things got even more challenging . Jess started to experience some really scary dark thoughts. Things felt hopeless and like there was no way forward. You might assume, as a psychologist Jess knew all about postnatal depression and how to get herself out of a funk, but knowing and doing are two very different things. Having a baby is different for everyone, and she just assumed she was more sensitive than others and it would pass. It just shows us that mental illness doesn’t discriminate, and it doesn’t matter who you are or what you know.
When things were at their peak, Jess found her own psychologist. Her GP put her on SSRI’s (antidepressants), and she took Rio to sleep school. Everything started to look up. Opening up to her closest friends helped Jess feel safe, and supported, despite being locked up (thanks COVID). Chatting to her partner was the hardest. She kept it close to her heart for so long as she didn’t want to put all the weight onto her husband as he was holding up her and Rio, while working full time.Jess said:
“People don’t tend to talk about their mental health, especially in the perinatal period as there is so much stigma. It’s meant to be this magical loved up time, so when you don’t feel that way you don’t want to admit it. I didn’t know anyone who had experienced PND/PNA so that was hard as I didn’t feel I could connect with anyone about the intensity of the struggle for me.”


There are so many options available such as pre and postpartum doula’s, lactation consultants, psychologists, sleep schools, PANDA phone counseling line, food delivery etc. Have your network ready to go. It seriously does take a village, but you have to set yours up these days.
If you need help, please contact PANDA or lifeline.